How to improve recovery from total knee replacement
A total knee replacement is a big operation, but it’s not as scary as people sometimes think. It’s almost bread and butter for surgeons and physiotherapists, so it’s important to feel comfortable with professionals who are well-versed in the latest research and developments.
While the majority of knee replacement surgery patients enjoy a positive outcome, we can’t guarantee it every single time.
To help you achieve a best-case scenario to optimise your pre-surgery fitness, body weight, pain and mobility, we also recommend a six-to-eight-week total knee replacement ‘pre-habilitation’ program.
PREFER TO LISTEN TO THIS ARTICLE?
We always encourage positive visualisation and documentation of the future here at The Physio Co (TPC). But don’t expect to be hopping out of bed and running home the day after a total knee replacement surgery.
That’s not to say the tennis career is over! Merely to say you’ll likely be watching the next major tennis tournament on TV rather than attending or participating at your local club – this year, anyway!
In addition to our six-to-eight week knee replacement surgery preparation guide, we’ve also created the step-by-step total knee replacement recovery guide below.
The following steps, recommendations and timelines are based on how our physiotherapists support knee replacement patients and help them reach their goals in roughly 8 to 12 weeks after surgery.
Day 0: The initial knee replacement recovery
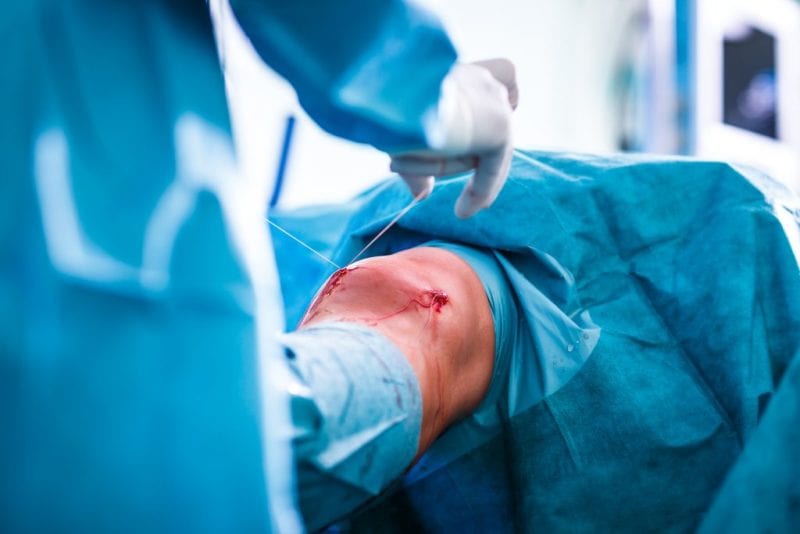
After a total knee replacement operation, you will likely wake up after 1½-2 hours under general anaesthetic. Your knee will be elevated, with a bandage covering the incision/s and possibly a drain to remove excess fluid from the joint.
The anaesthetic will leave your head feeling a bit foggy and the brain will be protecting the knee by avoiding movement.
Day 1: Weight-bearing, bending and a lot of ice
The very next day, our physios would be encouraging a patient to get up and about. We encourage weight-bearing (walking) and moving the joint through its full range, within the surgeon’s suggested limits.
While it’s not always possible, we encourage a target of 90-degrees bend. The main objective is to reduce swelling – so movement, elevation and a lot of ice.
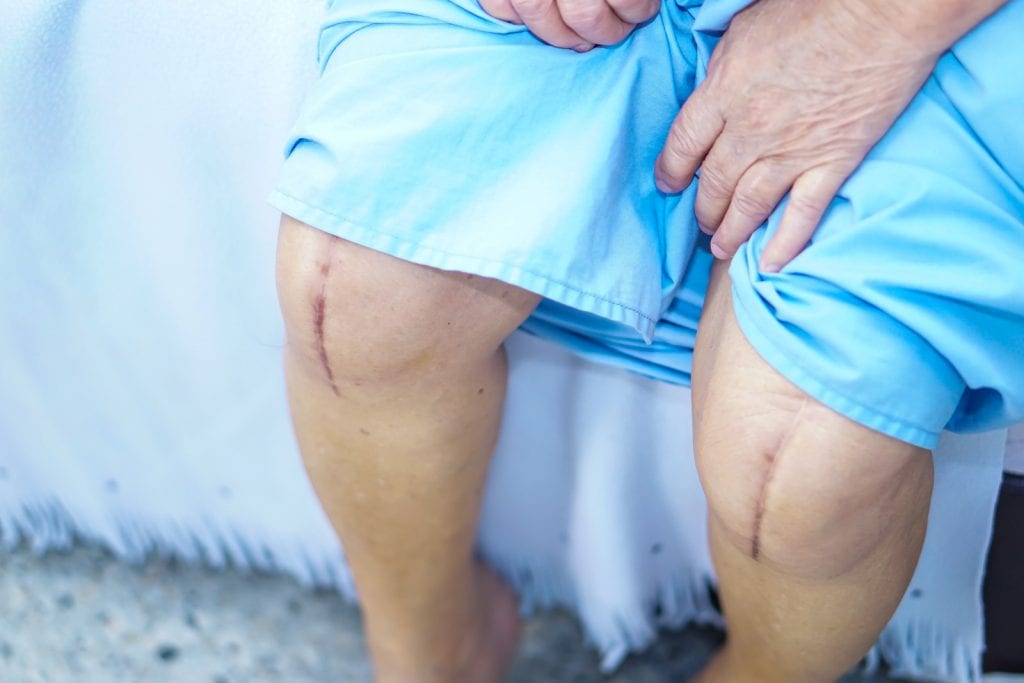
Days 2-5: Comfort and movement
Again, the key objective in this phase is to manage swelling and pain, while aiming for lots of good-quality movement.
It’s time to switch the muscle on and get some muscle activation without trying to build strength. Strength-based exercises can load the joint and contribute to pain, which we don’t want.
The whole leg will be swollen and there is likely to be bruising and discolouration around the ankle. As long as there is no real pain, there is no need to worry. If pain is localised to the bruising, let a health professional know immediately as it could be the blood clotting.
Please note: There will be pain or discomfort, after all, you’re not long out of a pretty big operation. We just need to make sure this pain or discomfort is at a manageable level.
Days 6-14: Strength throughout the whole range
For a knee joint, it’s essential to be able to get the leg straight. The natural tendency is to focus on bending, but an early straight leg suggests a positive long-term outcome. Surgeons usually like a straight leg!
Surgeons also like more than 90-degrees bend – a right angle or more – in being able to do functional things like sitting on a chair or getting on and off the toilet.
The joint will likely be swollen, so it is important to get that range of movement back as quickly as possible. This helps to get the blood flowing and reduce swelling.
Weeks 3-8: Loading the knee joint
Now we introduce more exercise-like movements such as squatting, as opposed to just swinging a leg.
Focusing on muscle activity during the pre-surgery period will have trained the mind to tell the leg what to do and, with a little prompting, the exercises should come back.

Week 8-12: The goal is in sight
It is possible to be up to doing a strength-based exercise program on your own after eight weeks.
If the initial goal has been ticked, then it can be time to set new targets around your mobility, independence and lifestyle.
No pain, no gain – just take the medicine!
There will be pain. There is no way around that, unfortunately.
At first, the surgeon will likely have you on some pretty strong pain relievers. As the swelling goes down, you start to move and get used to your new knee, the pain will usually get much less. We’ll help you monitor and manage your pain.
When the pain stops, we’ll stop using the painkillers because there is no other need to continue taking them.
It is really important that the surgeon’s pain relief program is adhered to in order to achieve mobility through rehabilitation without restriction due to pain. Regaining movement will help to reduce the pain and therefore work to end the medication program.
Avoiding medication by choosing to ‘tough it out’ or, using the medication for longer than you need it could lead to a delayed recovery.
It’s a joint effort to get the right pain relief with you and your medical team!
Interested in knowing more?
Please call on 1300 797 793 or contact our friendly physio team here today.



 1300 797 793
1300 797 793